Day +13 – Sunday
Feeling a bit down today – missing the kids and being at home and I’m feeling lethargic for the first time – was much brighter yesterday. I did a very short walk around the ward and found it a bit scary as was wobbly. All part of the roller coaster I was expecting and I think I’m still recovering from the shock of how quickly things went south the other night. For those interested I found a couple of papers on the intricacies of dealing with CRS in the clinical setting
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4929924/
http://hospitalhealthcare.com/latest-issue-2018/car-t-cell-therapy-managing-side-effects/
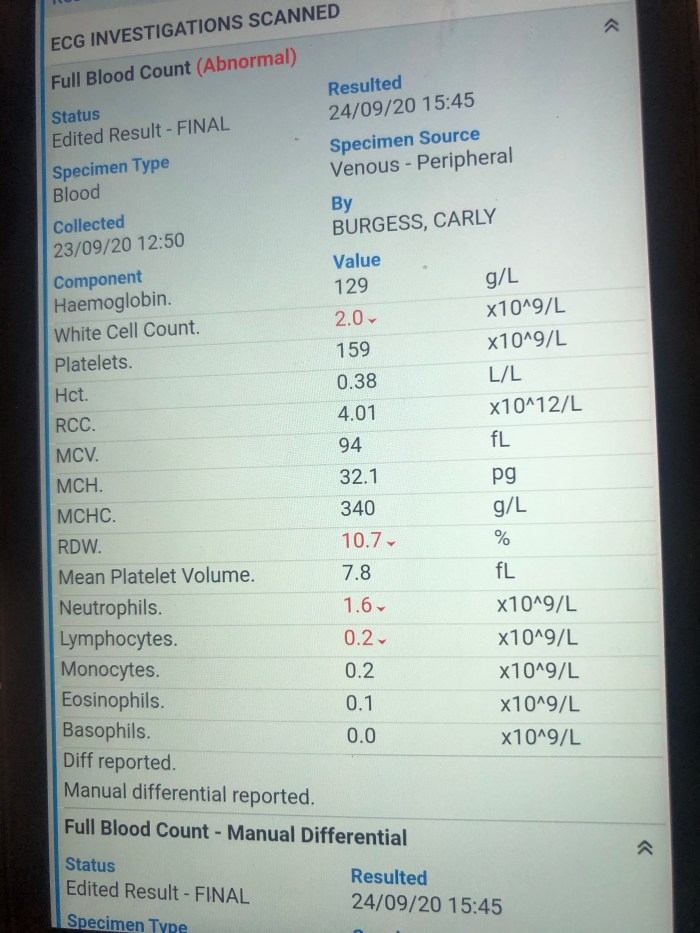
Dr Mary Ann Anderson came in especially to see me this morning – on a Sunday! She told me my neutrophils have fallen to 0.9 which is what they would expect at this stage and that my lymphocytes have risen to above 3 which is the first time they’ve been that high since I started venetoclax back in 2015. Lymphocytes are normally what they track to see cancer progression and I asked if it means the CAR-T is doing what ibrutinib does which is flushing them out of my bone marrow and lymph nodes into my blood stream and she said no her theory is that the rise is caused by the reengineered T-cell expansion itself but they just don’t know. We will know more about what’s going on 2 weeks tomorrow when I have my bone marrow biopsy to look for both the t-cells and any remnants of cancer.
In the meantime if my blood pressure stops falling I will be able to go home tomorrow but it’s more a you can rest at home because we trust you to come back quickly if you deteriorate than me actually being well. And Aideen pointed out she wasn’t expecting me to walk the Tan last time they let me out! Hello to her family in Ireland too who are following my blog while I remember.
Victoria has just shown me the bloods which Mary Ann discussed with me today. Here they are:
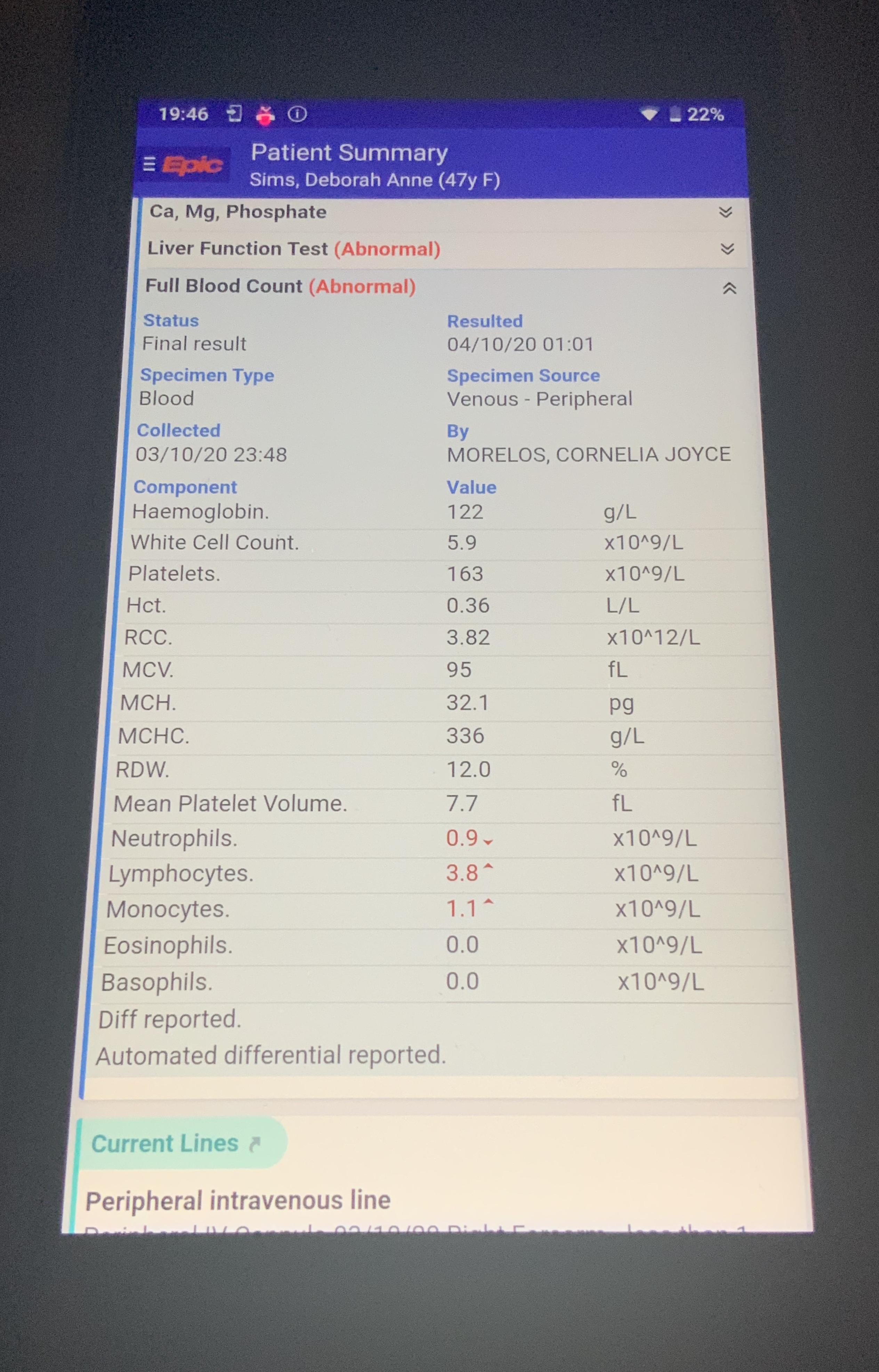
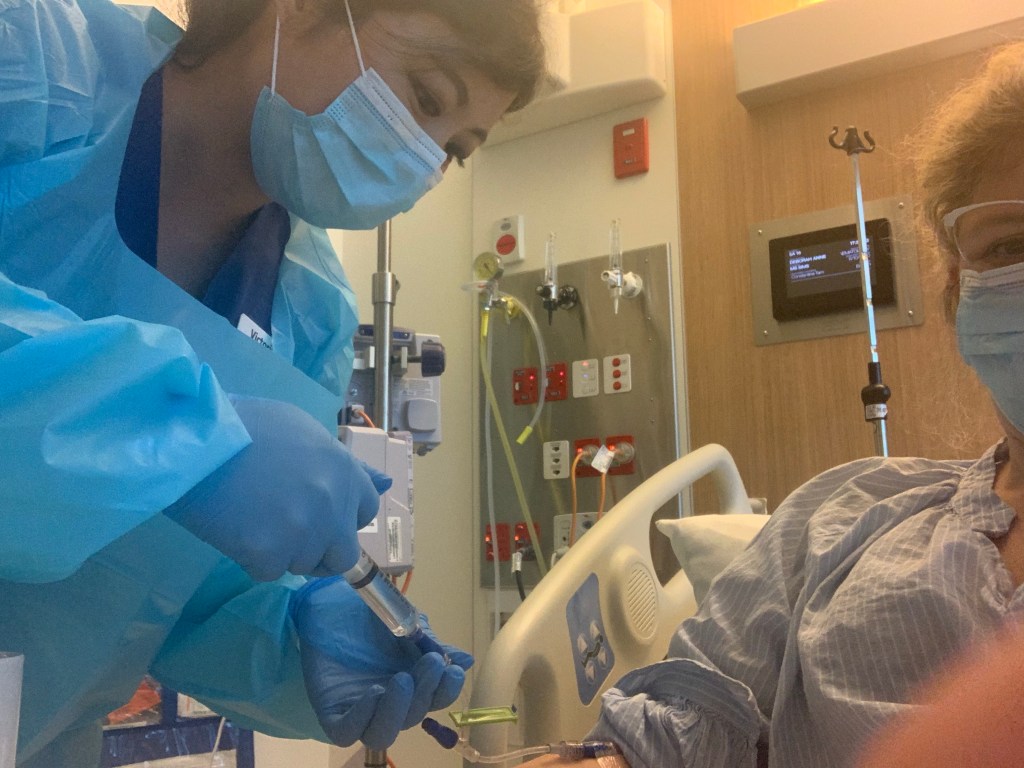
I had to get the canula removed from my elbow crease that emergency put in on Thursday night last night and it was almost a relief even being repricked because I hadn’t been able to bend my right arm for 3 days. But there are good sticks and bad sticks and you really learn to appreciate those who can canulate well. (I’ll try to keep this image small for the squeamish). Here’s what happened when someone missed the vein. And I have quite a few of that kind of thing that my poor arms have been subjected to over the past few days. I can see why I hear some cancer patients telling me how much they love their ports.
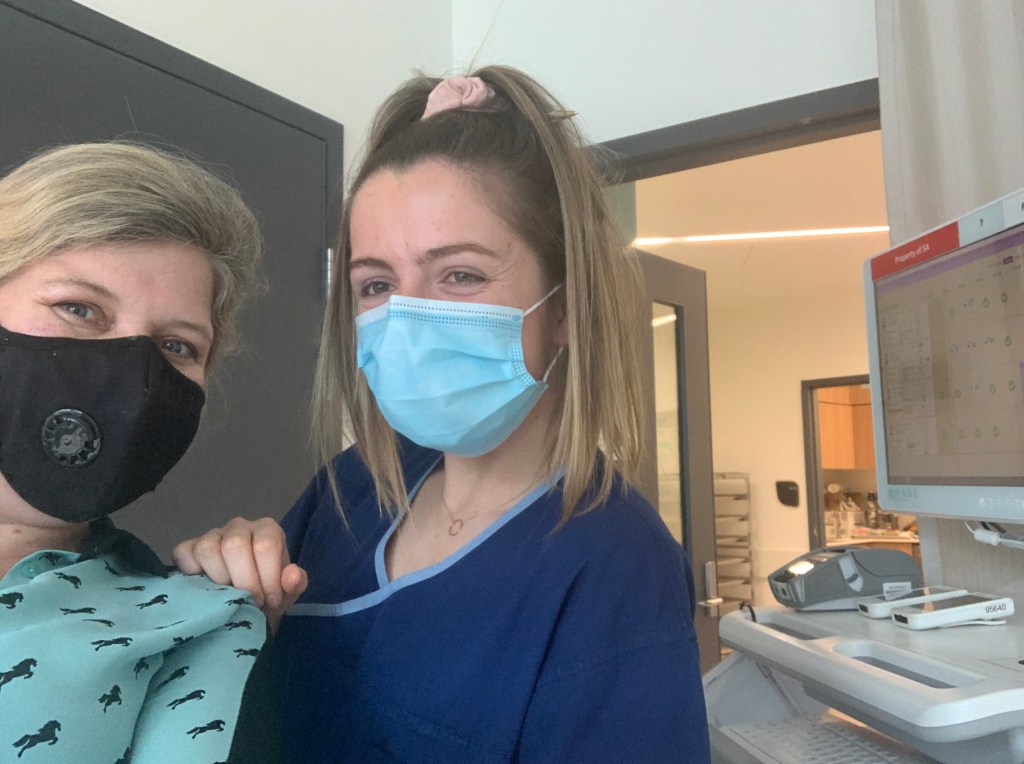
All part of the experience but you really appreciate the good sticks like Lia did for me last night. Lia is from the Philippines and has been working here for 3 years. She nailed it. She explained to me that in her home country patients have to pay extra for PICC lines and ports and most can’t afford it so they have to canulate patients with poor veins all the time. I’m enjoying learning about where they all come from. Wish I had been doing a featured nurse of the day from the start of this! I didn’t know that overseas nurses have to do a 3 month course and pay $16,000 to get their licence to practice in Victoria either regardless of how long they’ve practiced overseas.

Despite the massive differences in their cultural backgrounds there is definitely a strong cohesive Peter Mac culture here – I don’t know if it’s a combination of the building and management but I can’t imagine anywhere in the world doing it better so I’ll try to stop feeling down and enjoy it for hopefully the last night on 5A.